| | Life cycle of Taenia solium | How do you know if a pig is infected? | How can I prevent swine from becoming infected? | How does the tapeworm harm humans? | Can people be treated?
Cysticercosis is an infection caused by the pork tapeworm, Taenia solium. This parasite is found worldwide and is common in countries where raw or undercooked pork is eaten.
Although incidences of infection are extremely rare in Canadian and American swine herds, over 1,000 human cases of cysticercosis are reported annually in the United States. Many of these human cases result after travel outside Canada and the United States.
Life Cycle of the Taenia solium
The life cycle of the pork tapeworm follows a cyclic pattern:
- The cycle begins with swine eating food or drinking water contaminated with eggs from human feces.
- The enclosed larva in the egg is called the oncosphere. Oncospheres hatch in the pig's small intestine, penetrate the gut wall and move to a number of areas inside the animal.
- The oncosphere quickly changes into a fluid-filled bladder form called a cysticercus. Intramuscular sites are the most common place for cysticerci to develop in the pig.
- The cysticerci become visible within 2 to 4 weeks, and reach their full size in 60 to 70 days. The cysticerci remain infective in the pig for approximately two years.
- Cysticerci are passed from swine to humans via raw, undercooked pork or insufficiently cured pork or ham. Once in the human intestinal tract, they mature into adult tapeworms. Humans are the only host in which an adult tapeworm develops.
- The tapeworm attaches to the human intestine by its "head," called a scolex. The tapeworm grows to a length of 2 to 7 meters in 5 to 12 weeks.
- Most of the tapeworm consists of a chain of 700 to 1,000 segments. Each segment at the hind end of the chain is packed with up to 40,000 eggs. These egg-filled segments separate from the chain and are passed in the feces. These segments disintegrate in the soil, freeing the eggs, and renewing the cycle.
Humans can also be infected by accidentally swallowing tapeworm eggs. In these cases, the cysticerci develop primarily in the muscle, but can also infect the heart, eye or brain.
The pork tapeworm can live for over 20 years, producing several thousand eggs daily. One tapeworm can shed up to 300,000 eggs per day.
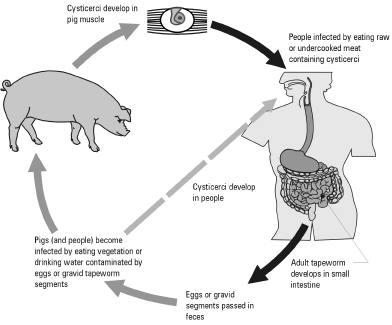
Figure 1. Life cycle of the pork tapeworm.
How do You Know if a Pig is Infected?
Pigs usually do not show signs of infection. A cysticerci infection (commonly referred to as measly pork or pork measles) is usually only found when the meat is inspected.
Cysticerci are found chiefly in the muscles of the swine heart, tongue, forearm, thigh and neck, but can occur in other parts of the body. Intramuscular sites are the most common areas affected.
How Can I Prevent Swine from Becoming Infected?
Food, water or soil may become contaminated with tapeworm eggs from human feces. Prevent exposure by:
- cooking pork thoroughly
- washing hands frequently when preparing food
- using clean utensils to prevent cross-contamination during food processing
- properly disposing of human waste thereby preventing the contamination of food and drinking water sources
Can other animals carry infection?
Cysticerci can develop in dogs and black bears. These animals act as reservoirs of infection by maintaining a supply of the infective source.
How Does the Tapeworm Harm Humans?
The presence of an adult tapeworm in the intestine may cause non-specific symptoms such as abdominal pain, diarrhea or constipation.
Cysticerci have been recovered from all areas of the body. Symptoms depend on the particular body site involved and the number of cysticerci present. The most serious consequences occur when the larvae develop in the brain, causing a condition known as neurocysticercosis.
Can People be Treated?
See your medical professional for treatment.
Prepared by:
Murray J Kennedy, Ph.D.
Food Safety Division
Source: Agdex 655-10. February 2005. |
|